There were no reports of infection.īlum et al. After initial debridement NPWT was applied and changed every 3-4 days for 11-29 days, 15 of the 16 patients healed by secondary intention (production of granulation tissue), a free flap was required in a single case. prospectively treated 16 patients with open wounds in the foot and ankle region demonstrating exposed tendon or bone. All patients healed without infection, one required a free flap.Īs a demonstration of the ability of NPWT to encourage the formation of granulation tissue over longer periods, Lee et al. They found a significantly reduced wound size in the NPWT group over the 8 days (mean 13.24 mm versus 3.02 mm, p=0.0001), a reduction in bacterial growth by day 8 (60% no growth versus 20%), and significantly increased angiogenesis, granulation tissue and fibrosis (Wilcoxon signed-rank test p<0.05). Each time the dressings were changed, measurements were taken and at day 4 and 8 post-initial debridement, tissue biopsies were taken for histopathological analysis. randomised 30 open musculoskeletal injuries to NPWT dressings changed every 3-4 days or standard dressings daily. Of the entire study group of 58 patients, 21 had either a rotational, free flap or skin graft but the infection rate in this group was not separately analysed.Ī further study by Sinha et al. The NPWT group showed significantly less infections than the control (0 acute and 2 delayed versus 2 acute and 5 delayed, p=0.024). 37 fractures were randomised to interval NPWT and 25 had standard fine mesh gauze dressing. studied 62 severe high-energy open fractures, all receiving an initial irrigation and debridement and returning to theatre every 48-72 hours until wound closure. 
By sealing the wound between sterile theatre visits, NPWT offers protection from nosocomial contaminants as well as promoting local wound perfusion and drainage.Ī number of studies have compared NPWT with WTD dressings in this setting. This is particularly relevant to open fractures with extensive soft-tissue injury with reported infection rates as high as 66%, mainly caused by nosocomial bacteria. It is these periods between operative interventions where NPWT is most commonly used and where it shows advantages over the standard wet to dry (WTD) dressings. Further debridement of tissue that subsequently declares itself non-viable may be required prior to healing by secondary intention with granulation tissue, wound closure or plastic surgical coverage. Careful haemostasis and coverage of all vital structures such as vessels or nerves prepares the wound for the application of NPWT. A subsequent careful debridement of non-viable tissue and contaminants followed by irrigation reduces the risk of infection. Following the British Orthopaedic Association Standards for Trauma (BOAST) and British Association of Plastic & Aesthetic Surgeons (BAPRAS) guidelines ensures that a thorough exploration of the wound is performed that facilitates diagnosis of the extent of damage. The primary surgical treatment of an open fracture must always start with thorough debridement and stabilisation of the fracture before addressing the soft tissue defects. NPWT dressings were first described in the medical literature for use with open fracture wounds. Published deep infection rates for open tibial fractures range from 8-12%. VAC negative pressure wound therapy semiocclusive membrane wounds.Open fractures are at risk of developing complications infection and nonunion are often the most common and can cause the most significant morbidity. Finally, vacuum-assisted wound closure therapy has been demonstrated to be efficient for various clinical settings, such as the management of diabetic foot ulcers, pressure ulcerations, chronic wounds, and skin grafts. 
These include NPWT with instillation therapy (NPWTi-d), different cleansing options, and application of NPWT on primarily closed incisions. 
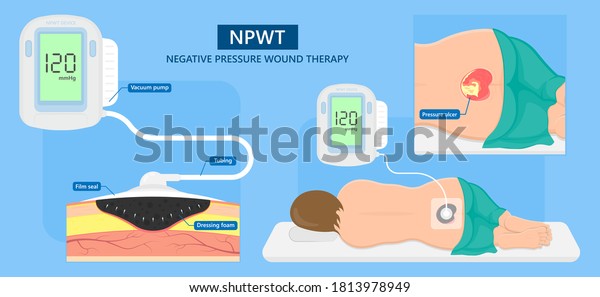
New NPWT modalities have been recently developed to make NPWT suitable for a wider variety of wounds. Rarely will complications linked to NPWT occur, but special care must be taken to prevent events such as toxic shock syndrome, fistulization, bleeding, and pain. Its effectiveness is explained by four main mechanisms of action, including macrodeformation of the tissues, drainage of extracellular inflammatory fluids, stabilization of the environment of the wound, and microdeformation. The system consists of a sponge, a semiocclusive barrier, and a fluid collection system. Negative pressure wound therapy (NPWT) promotes healing by evenly applying negative pressure on the surface of the wound.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
